Bladder Infections in Females: Why am I getting them?
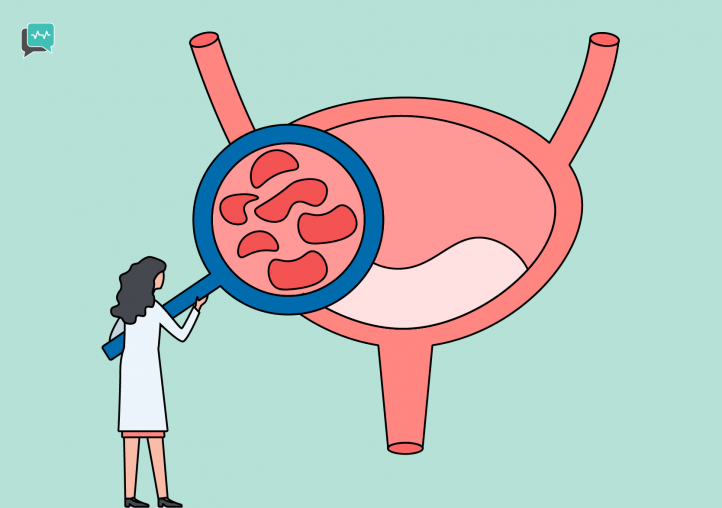
A UTI is an infection in any part of the urinary tract. Once the kidneys have made urine, the urine flows through the ureters down to the bladder where it is stored until a person urinates. At that point, the urine flows a short distance down through the urethra and out of the body.
The most common type of UTI in premenopausal women is an uncomplicated bladder infection. “Uncomplicated” means that there are no structural abnormalities or recent medical procedures that might predispose someone to bladder infections, and symptoms are limited to the bladder and urethra.
Uncomplicated bladder infections can affect anyone; however, women in their teens and twenties are particularly susceptible. Some studies have estimated that half of all female adults have had at least one UTI bladder infection during their lifetime. In common usage, the terms “UTI” and “bladder infection” are often used interchangeably.
Bladder infections that are treated with antibiotics rarely cause death or severe illness, but they can be very uncomfortable. Under certain conditions, untreated bladder infections can migrate to the kidneys where they can cause kidney damage and/or sepsis.
If left untreated, around 25% of bladder infections will resolve spontaneously.
What are the symptoms of a UTI?

- Symptoms of bladder infections in premenopausal women include:
- Pain or burning while urinating
- Lower abdominal fullness, discomfort, or pain
- Tenderness when an examiner presses on the bladder
- Need to urinate often or urgently
Less commonly, symptoms can include blood in the urine, fever, chills, and/or flank pain (pain towards the back, below the ribs). However, these symptoms are more typical of a UTI that has traveled to the kidneys, which requires immediate medical attention.
I am a healthy premenopausal woman. What is causing my UTIs?
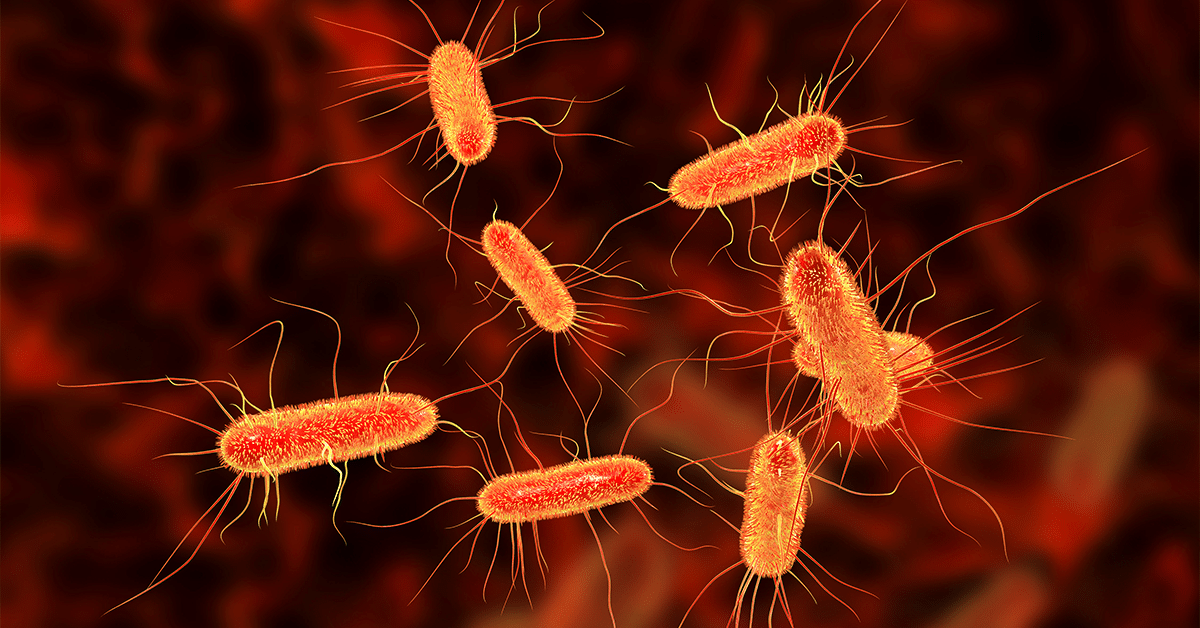
The most common cause of uncomplicated bladder infections in premenopausal women is E. Coli, a bacteria found in feces. E.Coli typically enters the bladder through the urethra and makes its way upward into the bladder.
What are the risk factors for bladder infections and UTIs? Can I change or minimize them?
You can modify some, but not all, of your risk factors. Risk factors include:
- Being female. Women have a relatively short distance from the anus to the urethra. They also have relatively short urethras. These short distances mean that E. Coli and other bacteria from feces are more easily spread towards the urethra and up into the bladder. Trans females who have had ‘bottom surgery’ are at risk for UTIs.
- A recent course of antibiotics for a different infection. In premenopausal women, the area between the rectum and the vagina, and the vagina itself, contain flora that help to suppress bacteria that is harmful to the bladder. A side effect of antibiotics is that they reduce this flora, which in turn allows harmful bacteria to grow. Because the urethra and the vaginal canal are so close to each other, the bacteria can spread from the vagina to the urethra and up into the bladder.
- Sexual activity. The activities during sex can spread fecal bacteria toward the urethra.
- Routine pelvic exams.
- The incidence of bladder infections is higher within the weeks following pelvic exams. Any sort of medical instrument in or near the urethra can raise the risk of infection.
- Age
- Although seen in women of all ages, bladder infections are most common in those in their late teens and their twenties.
- Pregnancy. Pregnancy increases the risk of developing bladder infections. The position of the growing uterus can restrict urine from flowing out. Any pregnant woman with a positive test of bacteria in her urine should be treated, even if she doesn’t have symptoms.

Can I do anything to prevent bladder infections?

- The acidity of healthy urine protects against bacterial infection. Organic acids from fruits and protein contribute to high acidity, so include them in your diet.
- Ask your doctor how much water it is safe for you to drink, and then drink that amount. Drinking a lot of water dilutes the concentration of bacteria in the bladder, and urinating helps to flush bacteria out of the urethra.
- Wipe from front to back after a bowel movement. Wiping from front to back helps to keep fecal bacteria away from the urethra.
- Choose a method of contraception that doesn’t require using a spermicide. Spermicides can reduce the flora that protect against harmful bacteria.
- Ask sexual partners to be mindful of the risk of spreading bacteria from back to front.
- Empty your bladder fully when urinating. Don’t “hold it in” if you feel the urge to urinate.
Why do my UTIs keep recurring?
Recurrent UTIs are defined as occurring 2 or more times within 6 months or 3 or more times within 12 months. In general, recurrent UTIs are actually new infections rather than a failure to cure the prior infection — even if the bacterial strain is the same one that caused the initial infection.
Unfortunately, recurrence is common, particularly when the initial infection was caused by E.Coli. This may be because E. Coli is relatively easy to transfer from the anus to the urethra. If you are having recurrent bladder infections, there are a few things you can do:
Ask the doctor to order a urine culture. The culture lets the lab look at which specific bacteria are in your urine so that you can be prescribed the most appropriate antibiotic. If you finished the full course of antibiotics and your infection recurred within a couple of weeks of the initial infection, it might mean that you did not have the right antibiotic.
Make sure to take the preventive measures outlined above.
If your infections aren’t responding to preventive measures, you can ask your doctor to refer you to a urologist for further investigation of the problem. Conditions that can make someone more likely to get UTIs include kidney stones or other obstructions within the urinary tract.
A few common misconceptions about bladder infections
Misconception: Cranberry juice helps cure bladder infections.
Fact: Cranberries contain a compound which prevents bacteria from sticking to the walls of the bladder. This might help to prevent bladder infections but there isn’t enough good scientific evidence to know for sure. Cranberry juice will not cure an existing infection.

Misconception: My lower abdomen really hurts, it burns when I pee, and my urine is cloudy and smelly. Clearly I have a UTI, so my doctor should prescribe antibiotics over the phone.
Fact: Any or all of your symptoms can be caused by other conditions that might get worse while you waste time treating a UTI that you don’t have.
Misconception: I can stop taking my antibiotic once I feel better.
Fact: You must finish the full course of antibiotics. Feeling better does not mean that the bacteria are gone. It only means that there are not enough bacteria left to cause discomfort. Unfortunately, bacteria reproduce. Not only might they reproduce enough to cause more discomfort; they might reproduce just differently enough and spread just enough so that the antibiotic you and millions of other people rely on won’t work anymore.
More info: Antibiotic resistance is an enormous, worldwide concern. Soon we will no longer have effective antibiotics against some common infections. Make sure to finish the entire course that was prescribed, and don’t buy or take antibiotics without a prescription.
Despite your best efforts at prevention, you might still develop a UTI. When diagnosed early, UTIs tend to be very annoying, mildly painful, and simple to treat. However, UTIs can become very painful surprisingly quickly. If you have symptoms of a UTI and your health care provider can’t get you in for a same-day appointment, consider going to a walk-in clinic. The hour taken out of your day will be well-worth preventing the discomfort or pain of a festering UTI.
How Halza can help?
Manage your family’s health easily with the Halza app. Store, track & share all of your child’s medical records to have them with you, wherever you go. Monitor your child’s growth and vaccination schedule as well as upload reports and doctor’s notes all with the Halza app. QuickShare a complete overview of you or your child’s health with any attending doctor in seconds, during emergencies or whenever you need.
Simplify your health journey with Halza.