What are Shingles?

Many of us have heard an older aunt or uncle, or grandparent warn us about shingles.
They might have said “I wouldn’t wish it on my worst enemy”. And while others might warn us about the pain of kidney stones, gout, or leg cramps, shingles is usually on people’s Top Ten list of common pains they hope to avoid.
Unfortunately, approximately 30% of people world-wide will have an episode of shingles.
[lwptoc]
What Is Shingles?
Shingles is a disease caused by the varicella-zoster virus. Varicella-zoster is the same virus that causes chicken pox. So why does it seem that younger people get chickenpox but not shingles, and older people get shingles but not chicken pox?
The answer is that the varicella-zoster virus (VZV) first causes chickenpox and later causes shingles.
This is because our immune systems can’t fully get rid of VZV. Although the chickenpox symptoms go away after ten days or so, a small amount of VZV genetic material remains in our bodies. This genetic material hides quietly near the spinal cord at the base of a nerve, often for many decades. When the virus reactivates, it causes shingles.
Who Gets Shingles?
Anyone who has had chickenpox is at risk for developing shingles.
Virtually everyone (99.5%) in the U.S who was born before 1980 was exposed to chickenpox and is, therefore, harboring latent VZV. In 1995, a very effective two-dose vaccine was approved for the prevention of chickenpox. In the U.S and some other countries, this vaccine is routinely given to young children.
Rarely, people who have had the chickenpox vaccine develop shingles as a result of latent VZV from the vaccine. The benefits of the chickenpox vaccination still outweigh the risks.
Requirements for the chickenpox vaccine and the availability vary by country.
Chickenpox vaccine can prevent from developing shingles
Other risk factors for developing shingles include:
- older age, although shingles is also seen in children
- not being vaccinated against chickenpox
- not being vaccinated against shingles if you have had chickenpox
- taking medications such as steroids, chemotherapy, or transplant-related immunosuppressives.
- having a weakened immune system
- having HIV
Anyone with these conditions should avoid being near someone with shingles. People with shingles should cover the rash and wash their hands frequently and avoid direct contact.
In the U.S., it is estimated that half of all people who live to age 85 will have had an episode of shingles. This is expected to decrease over time.
Why Do People Get Shingles?
We don’t know exactly why VZV reactivates in some people but not in others. Since it is most common in the elderly, one theory is that immunity drops off over time. Most likely it reactivates when your immune system is not working as well as it should, and the virus seizes an opportunity.
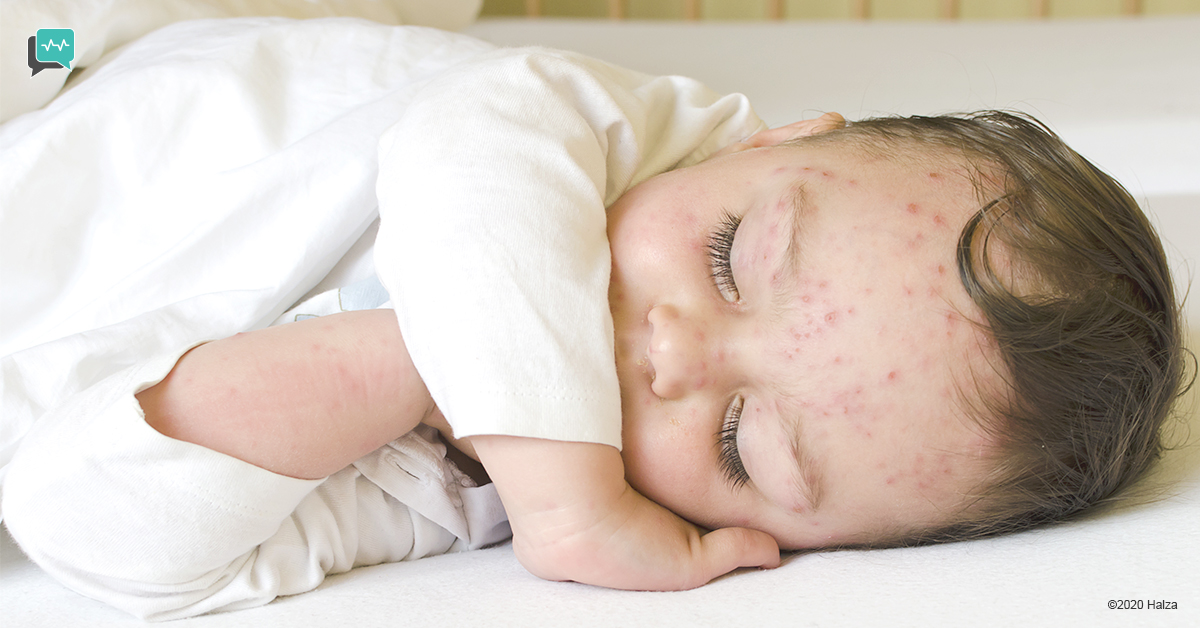
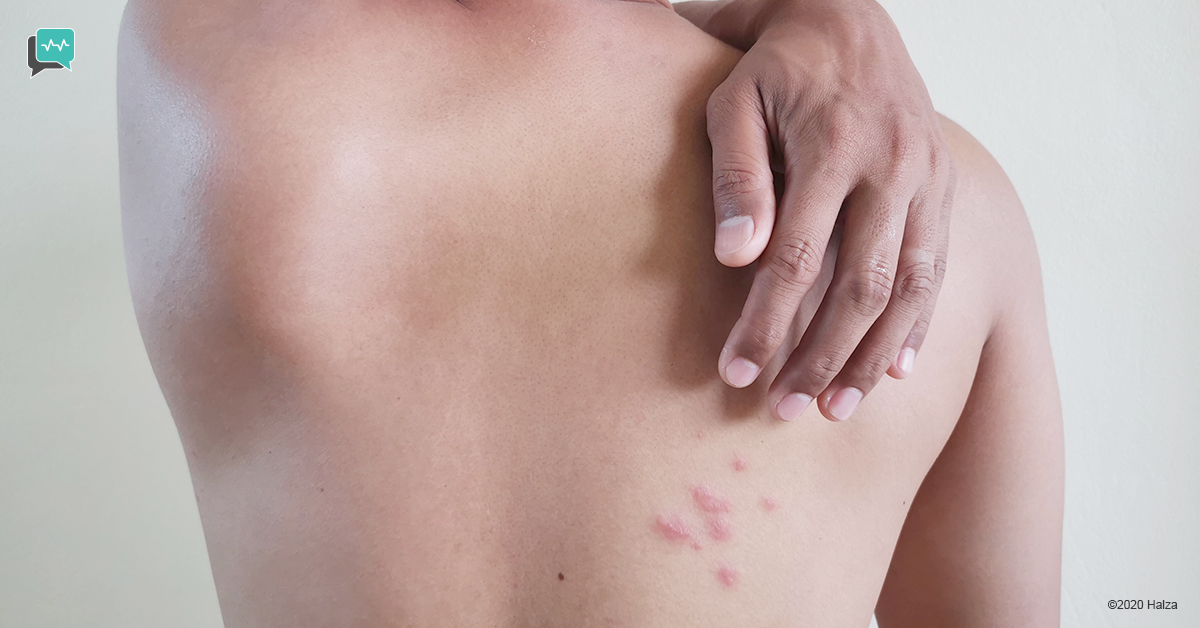
What Does Shingles Look Like?
Shingles looks like an angry red rash with many small, fluid-filled blisters. The blisters and redness are clustered together on either the right or left side of your body. This one-sidedness is important in diagnosis.
Although arms and legs can be affected, the most common areas include the:
- Neck
- Back
- Chest
- Abdomen
- Face/head/eyes
The rash appears only on one side because the virus reaches your skin by creeping along branches of a nerve that has ‘hosted’ the latent virus. Nerves branch out from either the left or the right side of your spinal cord. The area of skin affected by that nerve is called a “dermatome”. Some nerves wrap from the back to the front, causing a rash on the side.
What Does Having Shingles Feel Like?
The pain of shingles is described as:
- burning
- stabbing
- stinging
- sharp
The pain can be constant or sporadic. It tends to be worse at night and at rest.

Warning signs of shingles can occur before the rash develops or may last throughout the rash. These signs include:
- headache
- general feeling of being unwell
- warmth, numbness, tingling, itchiness, sensitivity to touch, or irritation in the area of the dermatome.
- chills and/or fever
- sensitivity to light
- pain that mimics symptoms of appendicitis, angina or sciatica
Over the next few days, the area will look red and rough or bumpy, and a few days after that, blisters develop.
The blisters will ooze virus-containing fluid. The fluid contains the transmittable virus.
After about 10 days, scabs form. When all the blisters have scabbed over, you can no longer transmit the virus.
Without complications, most people recover within 6 weeks. The disease does occasionally recur, but rarely more than once. And unfortunately, it can cause serious complications.
What Are The Complications Of Shingles?

Post-herpetic neuralgia
The most common complication is called post-herpetic neuralgia (PHN). PHN is long-term nerve pain lasting from three months to several years. It affects approximately 20% of people who have had shingles, but most recover in a year or so. Risk factors for developing PHN include:
- advanced age
- advanced age plus being female
- severe pain at the beginning of a rash
- a large area of skin involvement
- being immunocompromised
Herpes zoster Ophthalmicus
Approximately 8-20% of people will develop a complication of shingles that can affect the eye and cause blindness. Warning signs include headache, malaise, and fever at the onset of shingles, and/or pain on the forehead, the eye, or the top of the head. A blister on the tip or side of the nose is a sign that the nerve that affects the eye is involved.
You must begin treatment early in order to prevent vision loss.
Herpes zoster oticus (Ramsay Hunt syndrome)
This complication of shingles found on the face and near the ear can cause ringing in the ears, hearing loss, facial paralysis, vertigo, and altered taste perception.
Bacterial infection
Breaks in the skin from irritation and open blisters leave the skin and underlying tissue vulnerable to bacteria. If your immune system is not able to fight the bacteria by itself, you must take antibiotics in addition to antiviral therapy.

Motor neuropathy
If nerves that control movement are involved, the affected muscle will become weak and atrophy. Around 75% of people will gradually recover strength in the affected muscle.
Less common complications can include:
- pneumonia
- meningitis
- Guillain-Barre syndrome
- encephalitis
How Is Shingles Treated?
Shingles is mainly treated with antiviral drugs. Ideally, you start taking the drug within the first 3 days of the rash while blisters are still developing. Immunocompromised people can start the drug up to 7 days after the rash develops. Antiviral drugs include:
- valacyclovir
- famciclovir
- acyclovir
Your doctor might recommend other medications to help with pain, itching and skin irritation, although they are not curative. These include:
- Antihistamines such as diphenhydramine
- Topical numbing creams, patches, or drying lotions
- Anti-inflammatory drugs such as ibuprofen
Non – medicinal recommendations might include:
- Keeping the rash and blisters dry and clean
- Cold compresses
- Getting rest and sleep
- Wearing soft, loose clothing in natural fibers such as cotton
- Relaxation therapies
For severe acute shingles pain or for post-herpetic neuralgia your doctor might also recommend:
- A short course of corticosteroids
- Narcotic medication (opioids)
- Anti-convulsant medications to calm overactive nerves
- Tricyclic antidepressants to regulate chemicals involved in the brain’s processing of pain signals.
- Capsaicin patch
- Massage
- Acupuncture
- Therapy for depression caused by chronic pain
- Consultation with a specialist in neuropathic pain
How Is Shingles Transmitted?
Shingles, also known as ‘herpes zoster’, develops as a result of having had chickenpox at some time in the past.
Shingles itself is not directly transmitted from person to person. Instead, a person with shingles transmits the varicella-zoster virus (which causes chickenpox). The varicella-zoster virus is spread by airborne transmission (coughing, sneezing, etc) or by direct contact with the fluid from the blisters in a shingles/herpes zoster rash. Scratching or rubbing the blister releases the virus into the air where you can inhale it.
Once you inhale or touch VZV, you are at risk of getting chickenpox (not shingles) if you:
- have never had chickenpox and therefore are not immune
- have not been vaccinated against chickenpox
Months or decades later, you can develop shingles as a result of getting chickenpox.
Chickenpox is usually a minor illness in otherwise healthy children. However, it tends to be severe in adults and carries a risk of death, particularly in pregnant women, premature babies, and immunocompromised people.
Is There A Vaccine Against Shingles?
Yes, there is.
In the U.S. in 2017, a two-dose vaccine called Shingrix replaced Zostafax as the preferred prevention against shingles and the pain of post-herpetic neuralgia. If you have had Zostafax, it is safe to get Shingrex as long as you wait at least 8 weeks after the Zostafax injection.
Shingrix, which is approved in the U.S., China, Japan, Canada, the EU, and Australia, is recommended for healthy adults over age 50 who have had chickenpox or the chickenpox vaccine.
Shingrix is more than 90% effective at preventing shingles and PHN. It remains highly effective for at least 4 years. Shingles that develops in someone who has had the vaccine is likely to be mild.
Related reading:
Your older relatives were right.
Shingles is at best highly unpleasant and at worst, life-threatening. The key to minimizing pain and complications is to see your doctor at the first sign of shingles and to begin antiviral treatment early in the course of the rash.
Of course, preventing shingles is the best option.
If available and appropriate, get the Shingrix vaccine, and if that is not available, get Zostafax, because some protection is better than none. And avoid being near or touching unprotected people while you have blisters.
As miserable as shingles is for you, it might be far worse for someone else.
How Halza Helps
Vaccinations are essential in protecting us from preventable diseases.
But there are also many different types of vaccinations you need to get. If you have kids, keeping track of their vaccinations can also be also a handful.
To make remembering all these vaccinations and booster shots easier, look no further than the Halza app.
Record any vaccination you have already gotten and take note of those you have yet to get, according to the recommendation of your country of residence. Having easy access to the date you had the shot and the lot number of the vial is also great in the instance of any medical emergencies or incidences that might occur.
Store, track, share your medical data with Halza. Available in 26 languages, the app is also perfect for if you find yourself overseas and in need of medical assistance.