Can Sex Cause Cancer? The Answer is Yes

What are the first 3 words you associate with the word “Sex”?
What are the next 10 words? The next 50 words?
Are any of those words “Cancer”?
How Does Sex Lead to Cancer?
Having sex can lead to cancer through the transmission of the human papillomavirus, known as HPV. Although you might know that some subtypes of HPV cause genital warts, other subtypes are responsible for causing:
- 99% of cases of cancer of the cervix,
- almost all cancers of the anus,
- most cancers of the penis, vulva, vagina, and oropharyngeal area (the area around the base of the tongue, soft palate, tonsils, and throat).
As you might have guessed from the locations of these cancers, cancer-causing subtypes of HPV are transmitted through vaginal, anal, and oral sex.
Around 90% of all sexually active men and women have been exposed to HPV. If you are sexually active, there is a good chance that you have already been exposed. Most of the time, your immune system clears out the virus within a couple of years and you never know that you had contracted it. If your immune system does not clear the virus out, years later a pre-cancerous or cancerous lesion can form at the location of the virus.
Be aware of your risk factors for HPV-related cancers, including:
- An impaired immune system.
- Tobacco use.
- Having had many sex partners.
- A previous HPV infection.
How Can I Know If I Have Been Infected with High-Risk HPV?
Currently, only the cervix can be screened for HPV. No screening test for HPV exists for the anal, penile, vaginal, vulvar, and oropharyngeal areas. This means that in those areas you can’t know if you have a high-risk subtype of HPV until a visible or symptomatic lesion develops, which can take 10 years or longer – or might never happen.
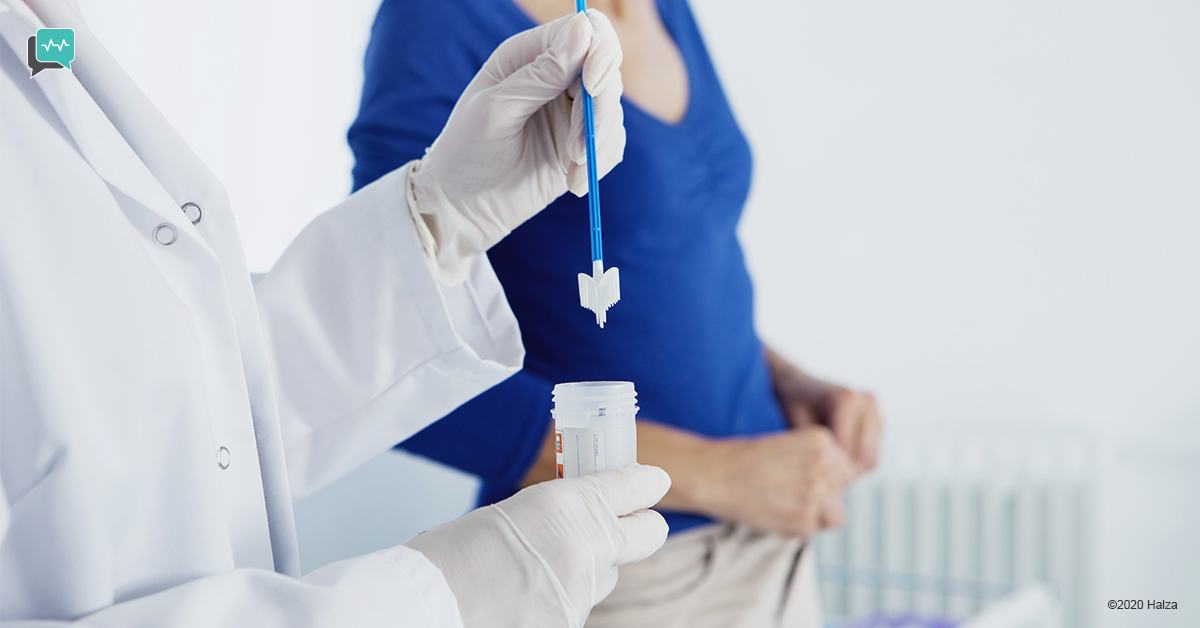
Cervical Cancer Screening
Globally, cervical cancer is the second most common cause of death from cancer in women, and in developing countries, it is the most common.
The HPV test is performed similarly to the Pap test and can be done at the same time as the Pap test. The difference is that the HPV test looks for the presence of cancer-causing HPV in cervical cells, rather than for actual changes to the cells. The HPV test won’t detect cancer itself, but it will identify women who have the virus and are therefore at higher risk of developing cancer.
What If I Have A Positive HPV Test Result?
A positive HPV test result does not mean that you will get cervical cancer, but you might need follow-up and more frequent testing.
HPV can be inactive for many years and not show up on an HPV test until it re-activates.

Anal Cancer Rates Are Higher Than Ever. What Should I Know?
If caught early enough anal cancer is usually curable with chemotherapy and radiation.
Risk factors for anal cancer – in addition to the risk factors for all HPV-related cancers – include:
- Receiving anal sex
- Receiving oral-anal sex
- Being HIV positive, particularly if not taking medication to prevent AIDS.
Signs and symptoms of anal cancer should always be checked by a doctor. These include:
- Bleeding from the anus or rectum
- Pain in or near the anus
- Anal itching
- A lump or growth in the anus
Even if a person doesn’t have symptoms, everyone with risk factors for anal cancer should raise the topic with their doctor. Discussing and checking for anal cancer is not typically part of a medical appointment unless the patient specifically expresses concern and asks to be checked. Since the anus is positioned fully inside the body, lesions can only be seen by a doctor.
Although there is no currently available screening test for HPV in the anus, a test similar to the cervical Pap test can be done to check for pre-cancerous or cancerous cells in the anus. This test can detect a developing lesion before it can be felt by the doctor. If your doctor does not have the necessary swab for this test, ask for a referral to have it done.

Oropharyngeal Cancer Rates Are Also Higher Than Ever
In the U.S., oropharyngeal cancer recently passed cervical cancer as the most common HPV-related cancer. Eighty-two percent of cases of oropharyngeal cancer occur in men, and most of these are caused by subtypes of HPV covered by the HPV vaccine.
Oropharyngeal lesions are in the back of the throat and may be difficult to see using a mirror. However, your doctor or dentist should look for lumps or lesions in your mouth and throat as part of a routine exam. Make sure that they include this at every checkup, including the base of your tongue.
Signs and symptoms of oropharyngeal cancer include:
- The sensation of a lump in the neck or throat
- An ongoing sore throat
- Lasting hoarseness
- Difficulty with swallowing
- Pain in the ear or jaw
- Swollen lymph nodes in the neck area
Now That I Know About HPV-Related Cancers, What Preventive Steps Can I Take Now?
Protect yourself by using a condom or dental dam during vaginal, anal, or oral sex. If needed, you can make one from a condom. For directions see https://www.cdc.gov/condomeffectiveness/Dental-dam-use.html
And get the HPV vaccination if possible.
Yes, There Is Actually A Vaccine That Can Protect Against Most Cases of HPV-Related Cancers!
The good news is that a vaccine is available in most developed countries that can prevent most cases of cancer caused by HPV. The older form of the vaccine, called Gardasil, protects against HPV subtypes 6 and11 (which cause genital warts), and high-risk HPV subtypes 16 and 18 (which cause most HPV-related cancers). Gardasil-9 adds protection against five additional cancer-causing subtypes.
Who Should Get the Vaccine?
The vaccine should be given before any form of sexual activity begins because it does not protect against any subtypes of HPV to which a person has previously been exposed. Without the vaccine, the chance of becoming infected with HPV from only one encounter with an infected person is very high.
In most countries, the recommendation is to vaccinate all males and females at ages 11-12. However, in the event that the vaccination is not given at ages 11-12, it can be given up to age 26. From ages 26-45 the vaccination is only recommended for people with specific risk factors who have not yet been vaccinated, and after age 45 it is not recommended.
Will Vaccinated 11-Year-Olds Think That Now It’s Ok To Have Sex, Or Have Sex Without Condoms?
Giving the vaccine doesn’t change anything parents should teach their children. It simply protects children from developing certain cancers.
- Condoms must still be used for protection. Gardasil only protects against the most common cancer-causing subtypes of HPV. It provides no protection against less common cancer-causing subtypes of HPV, or against any other sexually transmitted infections (such as gonorrhea, chlamydia, syphilis, or HIV).
Condoms provide only minimal protection against HPV and are not a substitute for the vaccine.
Why Should My Son Be Vaccinated?
Males should be vaccinated for several reasons:
- Anal and oropharyngeal HPV can be transmitted by oral sex, either heterosexually or homosexually.
- Although you might associate the vaccine mainly with preventing cervical cancer, in the U.S. oropharyngeal cancer has replaced cervical cancer as the most common HPV-related cancer. And 82% of people diagnosed with oropharyngeal cancer are male.
- If your son does happen to become infected with HPV, he can pass it on to other people, who may, in turn, pass it on to other people. Vaccination helps to break the chain of transmission.
- The vaccine also protects against genital warts, which can be transmitted through genital-area to genital-area contact.
- Side effects are minimal and are similar to those of other vaccines.
Put simply, this is a vaccine that can prevent common forms of cancer and save an untold number of lives.
Stay Healthy
Now that you know the connection between sexual activity and cancer, you can protect yourself – and your partner – from HPV. Keep your immune system healthy by practicing good nutrition and getting enough exercise and enough sleep. If you are eligible for the HPV vaccine, get vaccinated, and if you have children, have them vaccinated. Always be honest with your health care provider about your sexual practices and be sure that they examine any areas that concern you. If you have a cervix, be diligent about screening.
How Halza Helps
Managing HPV might mean undergoing many tests, consultations, and check-ups. It’s easy to let disorganization get the better of you. Let Halza help.
Instead of losing important reports and results, store all your medical records on Halza, including any Pap smear and anal cytology results, HPV tests, and colposcopy or biopsy data. All information is securely stored on Microsoft Cloud and belongs entirely to you.
Set Health Reminders for upcoming or recurring appointments to put your mind at ease and schedule Medicine Reminders to keep track of all your doses.
Download Halza today!
Sources: USPSTF – CDC – Cancer.org – ASHA – Cancer.gov