Dealing with Back Pain

Oh, my aching back…Most of us have some familiarity with backs.
For one thing, we all have one. And we all know someone who has a “bad” one – but what is a bad back, really? And how can you make sure that you don’t end up with one? Learn all about what contributes to back pain and how you can remedy the problem below.
What does a strong healthy back look like?

A strong healthy back has the following:
– vertebrae
The spine is made of 33 bones called vertebrae. The vertebrae are stacked one on top of the other in a way that forms natural curves. Together, the vertebrae carry most of the weight of the head and body. Maintaining the natural curves of your spine allows the weight to be distributed as intended.
– discs to absorb shock and enable movement
In between each of the top 24 vertebrae is a drum-shaped disc. The discs have a dense gel-like inner substance surrounded by a tough outer covering made of cartilage. These discs prevent the vertebrae from rubbing against one another. They also act as a slightly squishy sort of ball bearing between the vertebrae, allowing us to bend, straighten, twist, walk, and exercise in comfort.
– nerves to relay messages about movement and sensation to and from the brain
The spinal cord, a narrow, encased bundle of nerves, extends from the brain down through the vertebrae. At various points along the spine, individual nerves branch off at their root, exiting through small openings towards the rest of the body.
– ligaments to protect and connect
Ligaments connect the vertebrae and disks with one another, providing stability and protection.
– muscles to enable movement and provide strength and stability
Muscles connect the vertebrae to the shoulders, arms, pelvis, and ribs. They provide stabilization while enabling us to bend, straighten, and twist. Poor muscle tone and/or excess abdominal weight can pull the spine out of alignment. Poor alignment leaves the shock-absorbing discs vulnerable to damage from sudden or repetitive movements.
Additionally, poor alignment can, in turn, pull other areas such as the pelvis, hips, and shoulders out of alignment. Naturally, body parts connected with those areas will also be pulled out of alignment if the original misalignment is not corrected.
The back seems well-designed, so why does my back hurt?

The back is well-designed as long as we take proper care of it.
Most “bad backs” are a result of inflammation, arthritis, a strain or sprain, poor posture, pressure on a nerve, a fracture, or a combination of those things.
Discs can degenerate over time, simply through use and natural loss of moisture content. As discs wear out, the vertebrae can rub together causing inflammation, and eventually arthritis.
Bone spurs, often a result of arthritis, can grow and press on an adjacent nerve.
If any of the core muscles that provide support to the spine are weak – a common condition – just one wrong move, twist, bend, push, or pull can cause a small tear in the outer covering of a disc. This is particularly a risk if there is already normal age-related disc degeneration.
The gel-like interior of the disc “herniates” out through the outer covering. This condition is also known as a “slipped disc”. The covering itself has nerves which can be irritated. Depending on where the hernia is, the hernia can press on a nerve and cause pain. Interestingly, if the herniated area isn’t pressing on a nerve, you might not have any idea that you have a herniated disc.
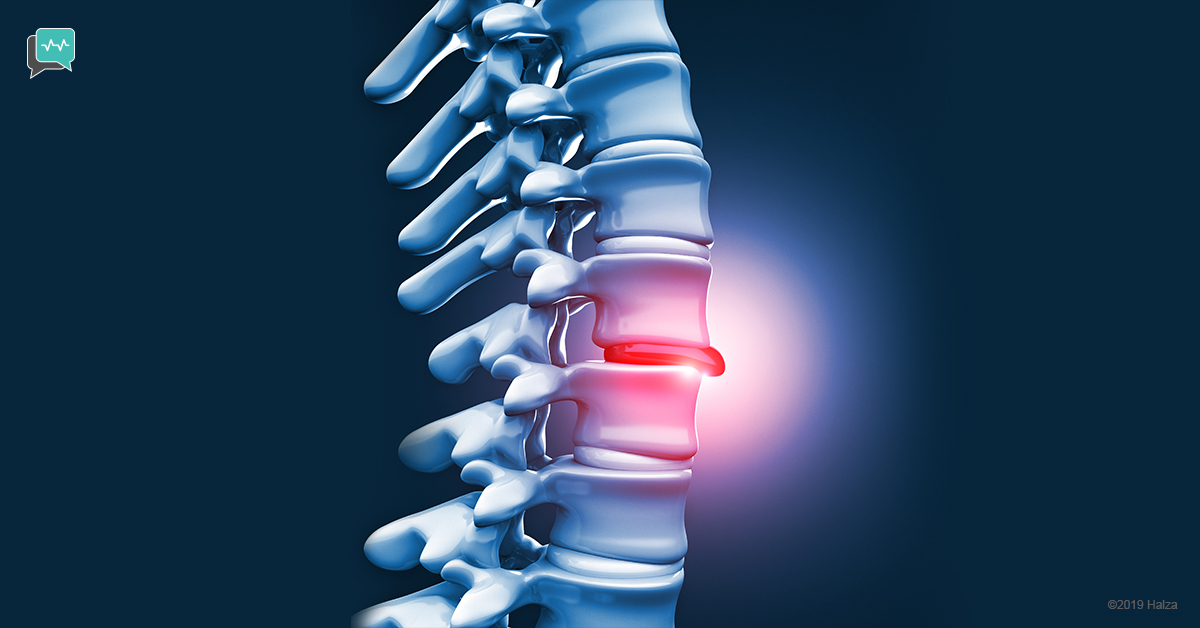
A milder form of a herniated disc is a bulging disc. The interior of the disc – still safely encapsulated – protrudes out from the beyond the drum-shaped portion of the vertebrae.
Vertebrae can fracture as a result of osteoporosis or injury.
In a condition called spinal stenosis, the parts of the vertebrae that normally protect the spinal cord become narrow, stiff, inflamed, and eventually press directly on the cord.
Whether from a bulging or a herniated disc, a bone spur, or spinal stenosis, if there is pressure on the sciatic nerve you will feel the symptoms of the dreaded but common sciatica. On each side of the body, the sciatic nerve branches out of the lower back through the hip and buttock, and then down the back of the leg. The symptoms described above can follow the entire length of the nerve or be limited to a small area.
Symptoms of pressure on a nerve vary, but include severe sharp pain, an electrical shock sensation, burning, tingling, and/or numbness. In extreme cases, there can be weakness and/or a loss of bladder or bowel control. These last symptoms require immediate medical treatment.
Why are back problems so common? It seems that almost everyone I know has back pain!

Bad backs are common for many reasons, some of which are not under our control. These include:
– age
– genetic predisposition to arthritis
– a curvature of the spine that developed in childhood (scoliosis)
– prior injury
– long-term courses of steroids
– growing up during famine
– having other diseases such as cancer
In addition to possibly having one or more of those conditions, we all usually have a fair amount of movement in our everyday lives. Moving the spine without having enough muscle strength and support is one of the biggest contributors to back pain.

Painful back conditions can often be prevented with some simple stretching and core strengthening exercises.
So, why shouldn’t I just sit still carefully at my desk all day, do a bit of low-impact aerobics, and then watch TV all evening?

Another cause of back pain is NOT moving.
– Slouching on a couch or hunching over a desk for long periods or sleeping on an unsupportive mattress all contribute to placing uneven pressure on the spine and wearing down the discs.
– Osteoporosis can lead to vertebral fractures. Weight-bearing exercise is an important factor in preventing osteoporosis.
– Excess weight contributes to misalignment. Movement can help trim off excess weight.
It can’t be emphasized enough that good core strength is an excellent way to prevent common back problems. Make sure to check with your doctor before beginning an exercise program, particularly if you already are experiencing back pain.
Other things that contribute to a healthy back include:
– having an ergonomic (user-friendly) workspace. Guidelines are available online.
– maintaining a healthy diet
– getting enough sleep so that injured areas can recover
– sleeping on a supportive mattress which keeps your spine properly aligned. There is no one-size-fits-all mattress recommendation – find a mattress that feels right to you.
– achieving an appropriate weight
– managing stress and tension, which can contribute to muscle strain.
– not smoking
– wearing comfortable, supportive shoes
– staying active and limber
Does back pain go away?
Yes, most back pain can be relieved through one or several methods. For the typical back-pain sufferer there is no instant cure, and you will have to follow a long-term treatment plan, but your pain will most likely diminish or disappear.
The sooner that you are able to begin treating your back pain, the better. Chronic pain, usually defined as lasting for three months or longer, is more time-consuming and difficult to address, but can usually be made quite manageable.
Your doctor might be able to diagnose the source of your pain through a physical examination, or she might recommend imaging studies such as an MRI, ultrasound, x-ray, or CT scan. In some cases, the doctor might recommend more specialized types of spinal imaging.
Newer studies indicate that the traditional advice to rest the back and stay in bed is in most cases, misguided. Most health care practitioners now recommend easing gently into movement as soon as possible after the initial injury or inflammation.
Treatment for back pain often includes:
– Ice or heat
– Massage
– Ultrasound
– Strength and flexibility exercises (physical therapy). If you have access to a swimming pool, ask your doctor or physical therapist about exercises you can do in the water.
– Pain control methods include: acupuncture, meditation, biofeedback, medication, electrical stimulation, injection of a steroid or an anesthetic next to the spinal cord (called an “epidural”)
– Back brace (some are available in pharmacies, but your doctor might recommend a more customizable brace)
– Counseling
– Surgery, but usually as a last resort. We recommend getting at least two opinions if not more before proceeding with surgery. Studies are mixed on the efficacy of several ‘mainstream’ spinal surgeries.
Alternative or complementary therapies, which might include herbs, spinal manipulation, a low-inflammation diet, yoga and/or tai chi.
A newer alternative option – for people whose doctors have found nothing wrong – is available through practitioners who treat Tension Myositis Syndrome (TMS). TMS describes a syndrome in which the brain substitutes physical pain in order to avoid feeling emotional pain.
The brain makes this substitution by reducing the flow of oxygen to the back or another area. The reduced oxygen level causes very real, not imagined, pain. Once the patient accepts that the pain exists only to provide a distraction from emotional pain, the patient can work their way through their repressed emotions. As a result of that process, the pain disappears.
If practitioners who treat TMS are not available, it is possible to work through the process yourself. Books like “Mind-Body Connection” by its founder, Dr. John Sarno, are widely available, as are workbooks by other practitioners.
Because there is no “quick fix” for most back pain, people may worry that their pain is permanent. Back pain can be awful, and it may take some time and effort to find the right treatment. But the reality is that treatment is effective for most people. Once fully treated, be sure to follow the suggestions for preventing a recurrence!
How Halza can help
Dealing with a chronic back condition is tough. Make life a little easier with Halza! Digitize and upload all your x-rays onto Halza and easily share the documents with any medical professional, whether chiropractor, kinesiotherapist, physiotherapist, or doctor. Keep track of any back-pain medication you need to take and set reminders for when you have to take them. If you find yourself overseas and in need of medical assistance, Halza is available in 23 languages. Communicate with your doctor and family via the app as well!
Sources: Johns Hopkins Medicine – AANS – Mayo Clinic
About the Author
Jill Sabin Garner received her Bachelor of Science in Nursing (summa cum laude) from New York University. A Registered Nurse and Certified Diabetes Educator, she serves on the boards of both the New York State Coordinating Body and the Metropolitan New York Group of the American Association of Diabetes Educators.